Closing Ohio’s health gaps:
Moving towards equity
HPIO is hosted an equity messaging forum on Thursday, Oct. 25, 2018, to explore how to tailor messages about health issues, particularly those impacting our most marginalized communities, to appeal to a broader set of Americans. See presentation slides from the event:
- Defining health equity and understanding health disparities in Ohio
Reem Aly, Vice President, Healthcare System and Innovation Policy, HPIO - A closer look at how Americans view health equity
Larry L. Bye, Senior Fellow, Health Care, NORC at the University of Chicago - Appealing to your audience: The importance of messaging
Sandra Harbrecht Ratchford, President and Chief Executive Officer, Paul Werth Associates, Inc. - Advancing health equity through messaging and communication
Nicole Bronzan, Senior Communications Officer, Robert Wood Johnson Foundation
Ohio has troubling health gaps
• There is more than a 29 year gap in life expectancy at birth depending on where a person lives, ranging from a low of 60 years in the Franklinton neighborhood of Columbus (Franklin County) to a high of 89.2 years in the Stow area (Summit County).
• Black infants are nearly three times as likely to die in the first year of life (15.2 infant deaths per 1,000 live births) compared to white infants (5.8 infant deaths per 1,000 live births).
• Ohioans with disabilities are four times more likely to experience depression compared to Ohioans without disabilities.
• Ohioans with less than a high school education are 2.7 times more likely than Ohioans with some post-high school education to report fair or poor health.

Why does this matter?
Ohio has seen worsening health outcomes and an increase in healthcare spending relative to other states over the past few decades. Ohio ranks 46th out of 50 states and D.C. on health value, based on the Health Policy Institute of Ohio’s 2017 Health Value Dashboard. This means that Ohioans live less healthy lives and spend more on health care than people in most other states.
Improving health value in Ohio means closing Ohio’s troubling health gaps and ensuring that every Ohioan has the same opportunity for a healthy life.
What is health equity?
HPIO convened an Equity Advisory Group to come to consensus on a definition of heath equity. The group reviewed existing definitions of health equity and developed the following: Everyone is able to achieve their full health potential. This requires addressing historical and contemporary injustices and removing obstacles to health such as poverty, discrimination, and their consequences, including powerlessness and lack of access to good jobs with fair pay, quality education and housing, safe environments and health care.
Why do we have health gaps in Ohio?
Making healthy choices (i.e. health behaviors) is critical for good health. These choices are often shaped by the social, economic and physical environments in which a person lives (see figure 1). Because of this, many Ohioans face barriers to being healthy. For example:
- Unequal access to education and Black children in Ohio are more likely to attend high-poverty, under-resourced schools with lower graduation rates. Lower educational attainment leads to limited job choice and often lower-paying jobs that offer fewer employee benefits, such as health insurance coverage.
- Poor neighborhood Low-income Ohioans often cannot afford to live in high-income neighborhoods. They are more likely to live in neighborhoods that report high rates of crime and violence and have difficulty finding safe places to exercise and play.
- Lack of public A family without a car in a city without adequate public transportation may have difficulty getting to the grocery store to purchase nutritious foods. Poor nutrition is a risk factor for a number of health conditions including diabetes, heart disease and preterm birth.
Many Ohioans also face the enduring consequences of racist and discriminatory historical and contemporary obstacles to health, such as slavery, Jim Crow, residential redlining and predatory lending.
How can we close Ohio’s health gaps?
Closing Ohio’s health gaps requires a comprehensive approach with public- and private-sector stakeholder collaboration. Figure ES.1 provides a five-step framework for action to achieve health equity at the community level. See the full brief for examples of evidence-based strategies and partners to achieve equity.
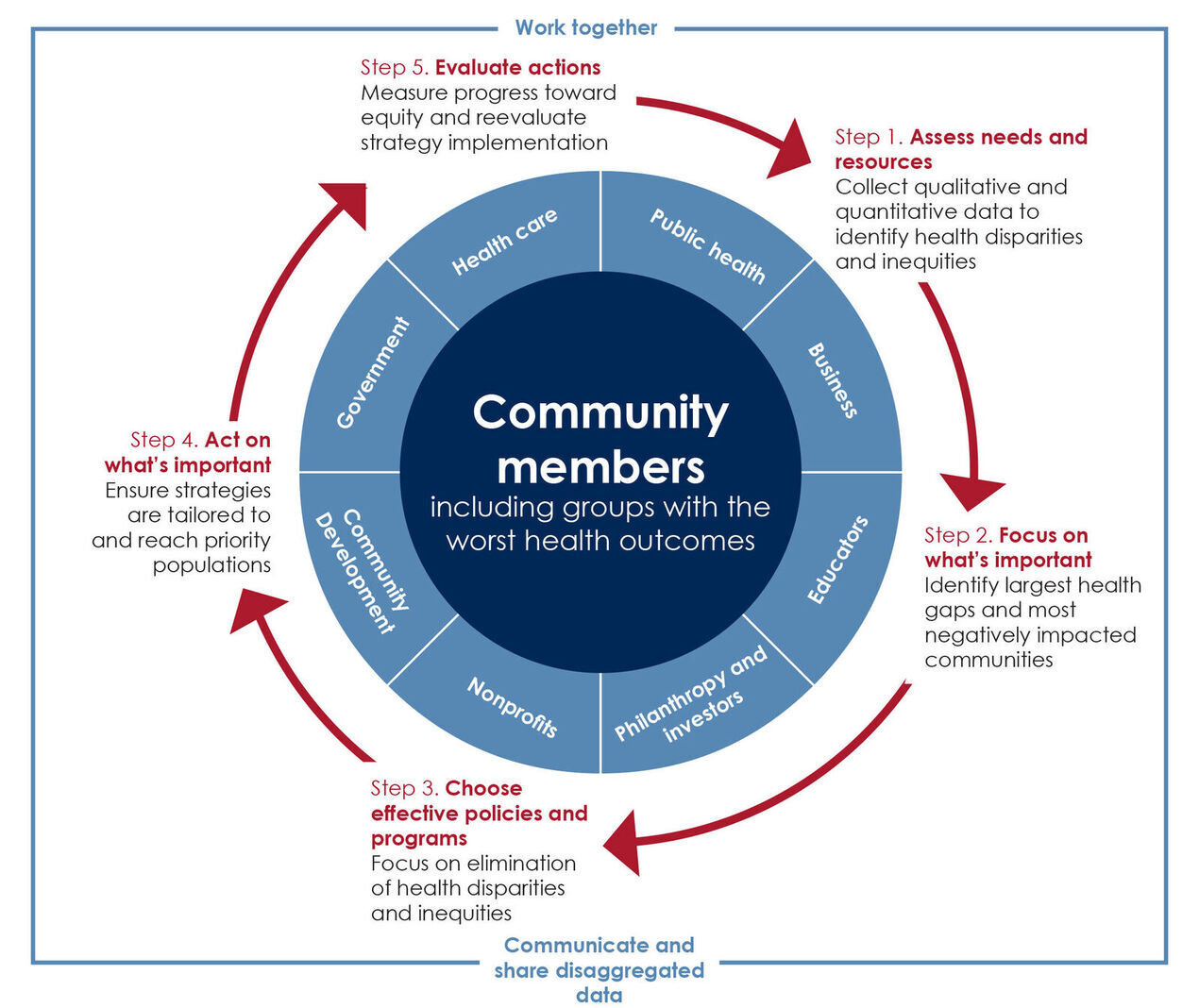
Source: HPIO adaptation of County Health Rankings and Roadmaps Action Cycle

